CREDENRO™ By VANAA
Provider Profiles Validated And Submitted In 24 Hours.
CREDENRO™ centralizes everything, auto-fills applications, and submits to payers
while you focus on actual
credentialing decisions.
Welcome Back 👋
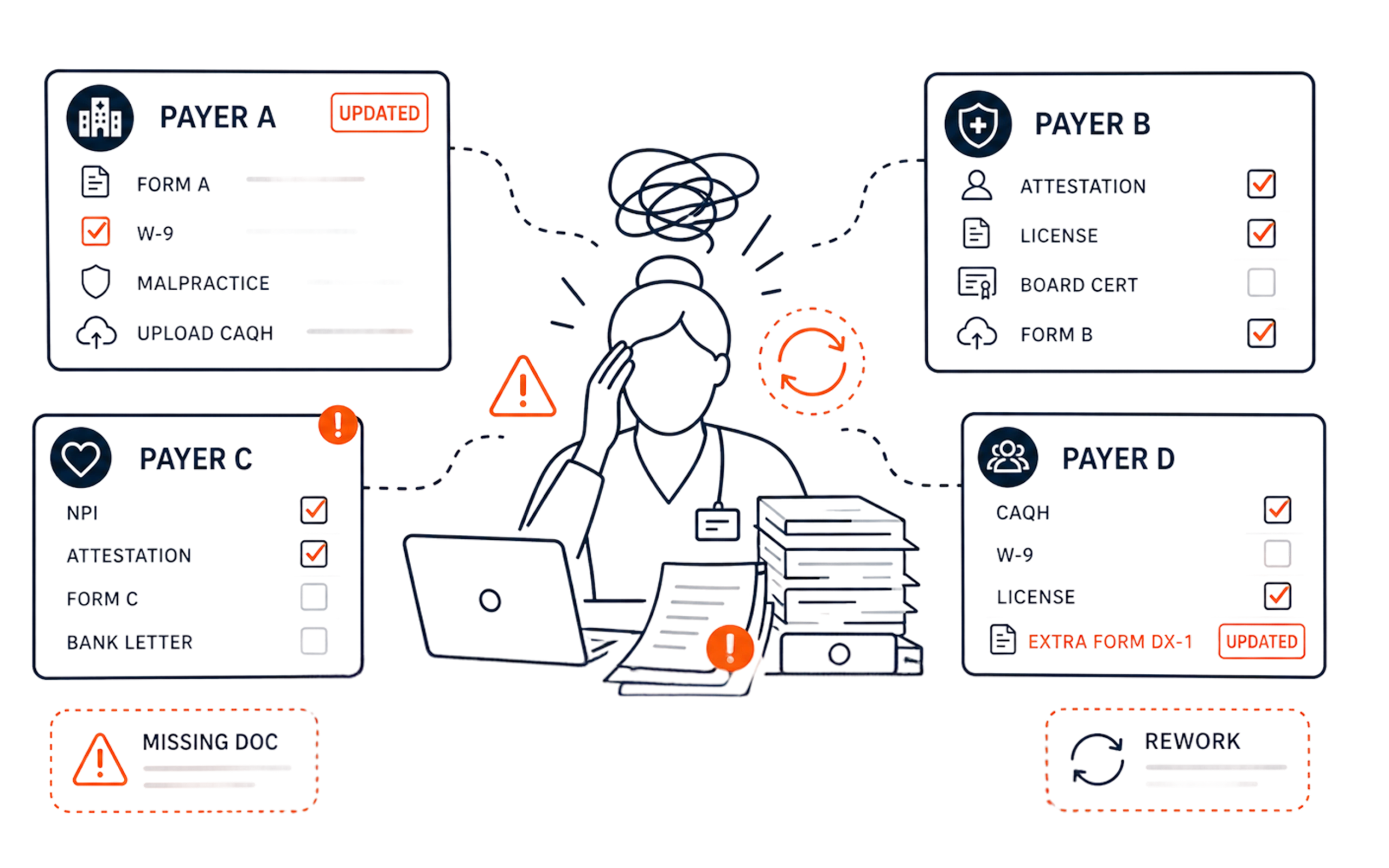
Fragmented Data, Payer-By-Payer Nuances, And Manual Renewals Create Systemic Risk.
Provider Data Chaos
HR has one version of provider licenses. CAQH has another. Your credentialing file has a third. Nothing is complete in one place.
Single source of truth syncs with NPPES, state boards, CAQH in real-time. Updates push back to external databases automatically.


Expiral Slippage
Licenses, DEA, PLI, and credentialing renewals expire on different schedules. Deadlines get missed. Claims denied. Providers de-networked.
Automated renewal calendar tracks every expirable. 90-60-30 day alerts. Auto-triggers re-submissions. Zero lapses.
Payer-Specific Requirements
Each payer wants different forms, different documents, different attestations. Requirements change without notice.
Intelligent payer rule engine recognizes provider license type and maps to correct enrollment path. Adapts when payers change requirements, no manual spreadsheet updates.
Eliminate Errors &
Grunt Work
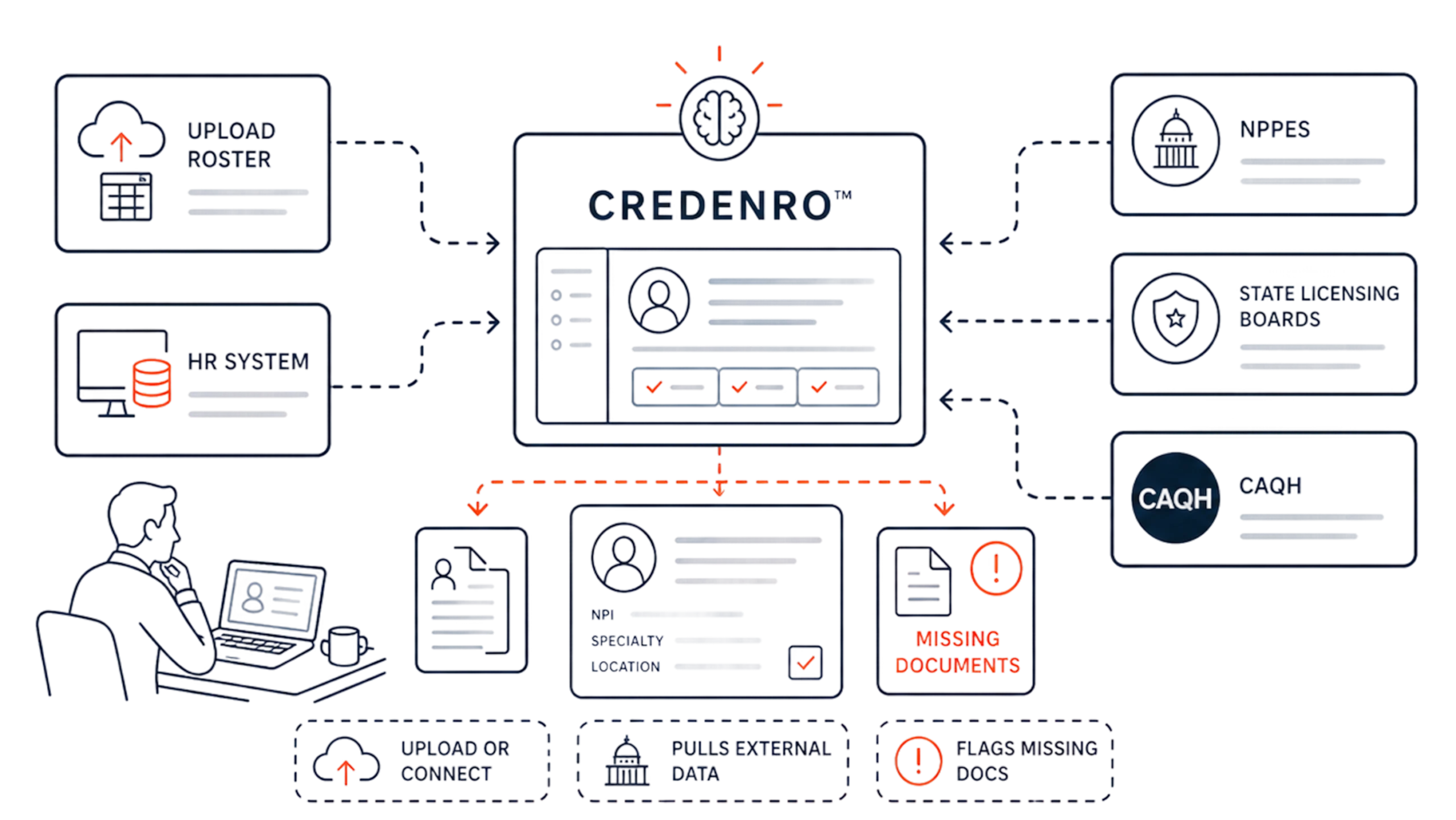
Import Provider Data
Upload roster or connect HR system. CREDENRO™ pulls info from NPPES, state licensing boards, CAQH. Flags missing documents.
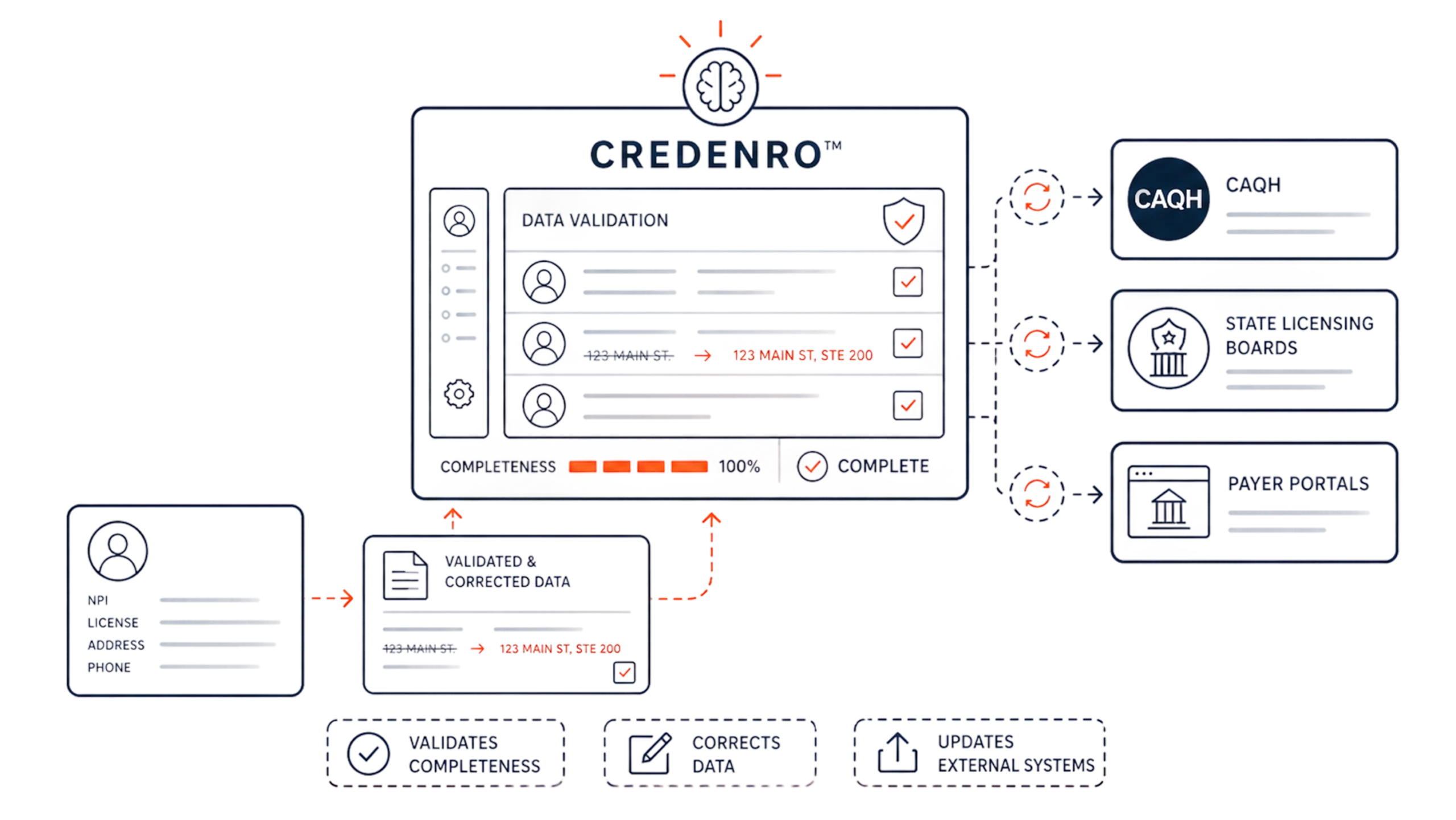
Validate & Update External Databases
System validates completeness. Pushes corrected data back to CAQH, state boards, and payer portals.
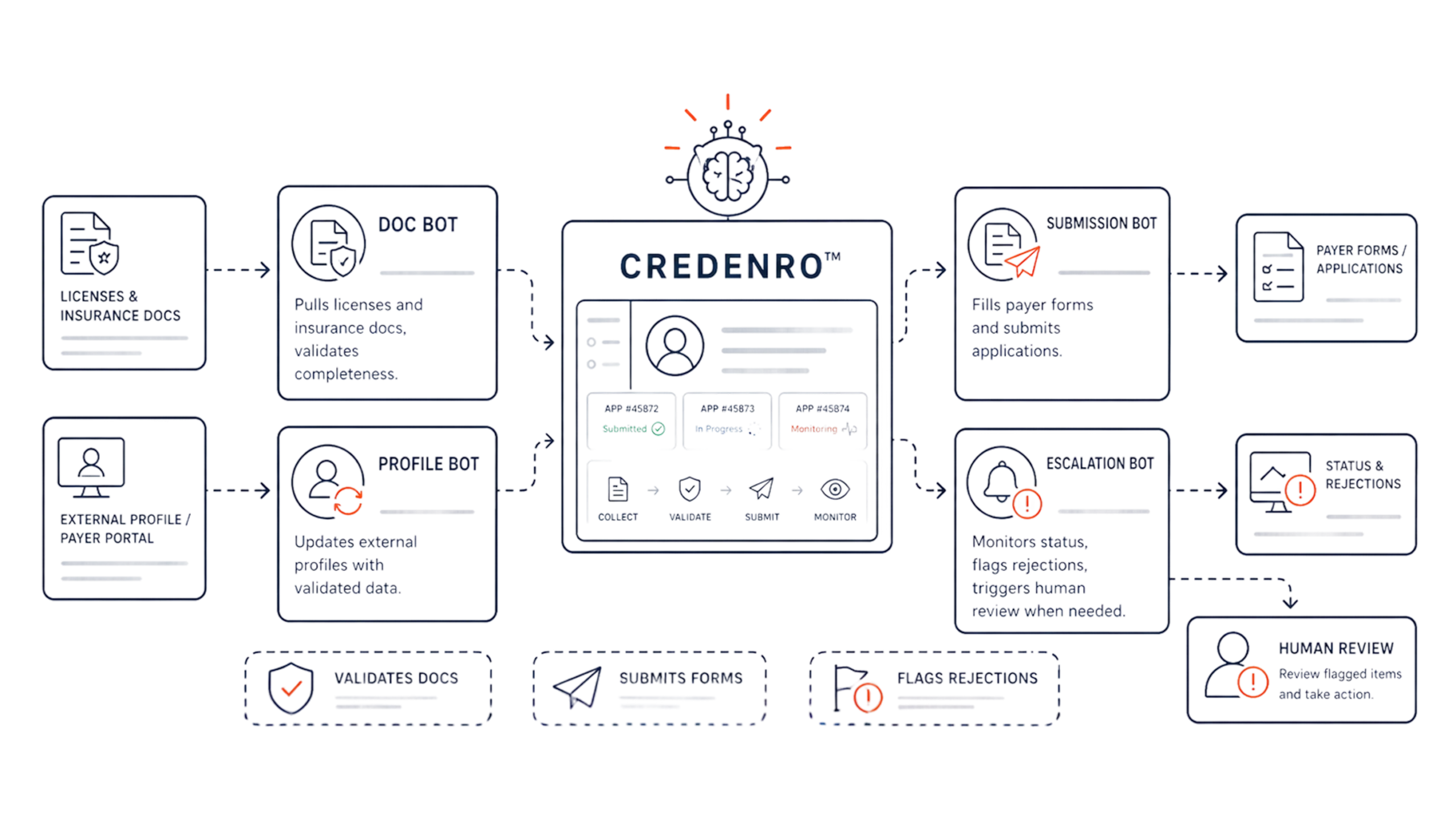
Auto-Submit Applications
4 bots handle the work:
~ Doc Bot: pulls licenses, insurance docs, validates completeness
~ Profile Bot: updates external profiles with validated data
~ Submission Bot: fills payer forms, submits applications
~ Escalation Bot: monitors status, flags rejections, triggers human review when needed
Result: 90%+ of enrollments submitted without manual intervention.
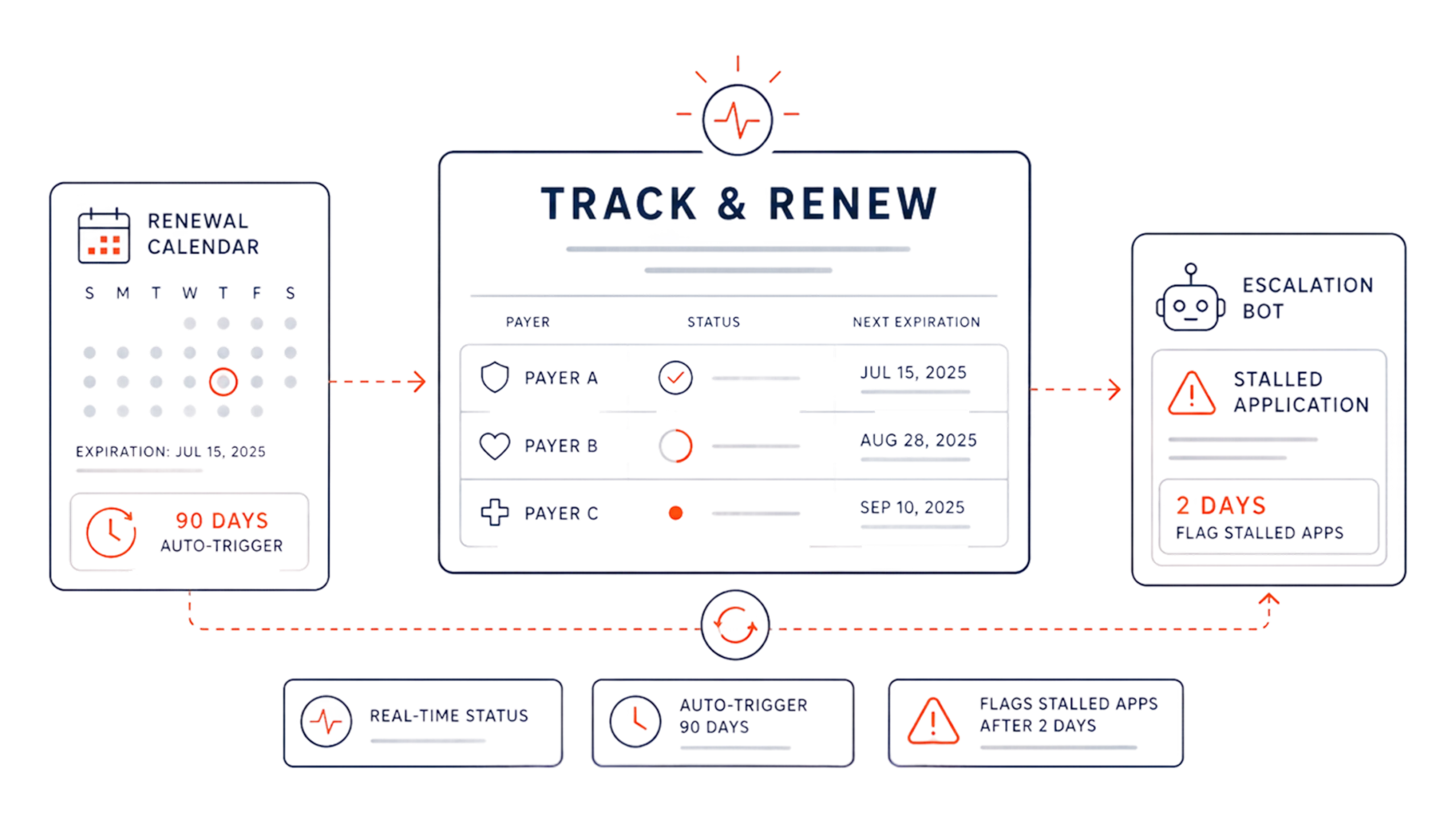
Track & Renew
Real-time dashboard shows provider status with each payer. Renewal calendar auto-triggers resubmissions 90 days before expiration. Escalation bot flags stalled applications after 2 days.
One Stop Provider Database,
Real-Time Connectivity
Enterprise-Grade Credentialing Security
HIPAA Compliant
All provider data encrypted. Access logged. Audit-ready.
CMS & Payors Rule Alignment
Application pathways based on keep changing for various specialties. Here they are updated within 24hours.
SOC 2 Type II
Enterprise-grade security and data handling independently verified.
Who Is It For?

Credentialing & Enrollment Companies
Managing 100+ active cases across 20+ payers without automation means endless form-filling and spreadsheet updates.
Bots handle data entry. Automated calendar prevents renewals from slipping. Ticketing system prevents chaos.

Healthcare Organizations / Startups
New providers wait 90+ days to start billing. Network growth slows. Revenue delayed
Parallel submissions. 35% faster onboarding. Proactive escalations when applications stall.

Providers
You're ready to see patients, but credentialing delays keep you off the schedule and out of network. Revenue is on hold while paperwork drags on.
Clear visibility into status, faster enrollment with payers, fewer "Provider Not Found" denials, and a predictable path to being in-network and billable.

Credentialing & Enrollment Companies.
Managing 100+ active cases across 20+ payers without automation means endless form-filling and spreadsheet updates.
Bots handle data entry. Automated calendar prevents renewals from slipping. Ticketing system prevents chaos.

Healthcare Organizations / Startups
New providers wait 90+ days to start billing. Network growth slows. Revenue delayed
Parallel submissions. 35% faster onboarding. Proactive escalations when applications stall.

Providers
You're ready to see patients, but credentialing delays keep you off the schedule and out of network. Revenue is on hold while paperwork drags on.
Clear visibility into status, faster enrollment with payers, fewer "Provider Not Found" denials, and a predictable path to being in-network and billable.
✦ TESTIMONIALS ✦ At Pure Psychiatry Group and ACPC, we are pleased to provide our strong endorsement of Vanna for their exceptional revenue cycle management and credentialing services. Since partnering with Vanna, including their credentialing department, we have experienced significant improvements in both our billing operations and provider onboarding processes. Their team consistently demonstrates a high level of expertise, accuracy, and responsiveness in managing claims, reducing denials, accelerating reimbursements, and ensuring timely and efficient credentialing with payers. As a result, our organization has seen measurable improvements in cash flow, operational efficiency, and speed to service for new providers. Vanna’s proactive approach and deep understanding of behavioral health billing and credentialing, including Medicaid and commercial insurance, have made them a valuable and trusted partner. We highly recommend Vanna to any healthcare organization seeking a reliable and knowledgeable revenue cycle and credentialing partner. Bridgette Trader Revenue Cycle Management Director Pure Psychiatry Group and ACPC Working with this billing company has been one of the best decisions I’ve made for my practice. Not only did they help recover revenue that was previously lost with another billing service, but they have increased our overall collections by approximately 26%.
Their communication is exceptional—they stay in touch daily, provide clear updates, and are always proactive in addressing any issues. What truly sets them apart is their team-oriented approach. They genuinely feel like an extension of our clinic, always positive, responsive, and invested in our success. They don’t just “do billing”—they truly partner with you and care about your growth.
Because of their dedication and expertise, we’ve been able to focus more on patient care while having full confidence that our billing is being handled efficiently and accurately. I highly recommend them to any practice looking to improve both revenue and workflow Susan Graham Owner and Nurse Practitioner, Hometown Healthcare Solution We’ve been working with Vanaa since 2024, and the impact on our revenue cycle has been immediate and substantial. Prior to transitioning, we worked with another billing company that unfortunately cost us a significant amount of lost revenue.From the moment Vanaa stepped in, they quickly identified missed opportunities and successfully back-billed tens of thousands of dollars that we had previously written off. Within just a few months, we saw a large influx of recovered payments that made a meaningful difference in our operations.Beyond their results, their responsiveness sets them apart. In addiction medicine, timing is everything, and Vanaa’s team is consistently quick, communicative, and proactive. We finally feel confident that our billing is being handled with urgency and expertise. Derek Bravo CFO, Renew Health The credentialing team has been exceptional to work with. Their knowledge of payer requirements, timelines, and processes is far beyond any credentialing or management team we’ve worked with in the past.They’ve implemented efficient systems and clear procedures that make onboarding providers smooth and predictable. As a result, our providers are getting credentialed and ready to see patients much faster.Their ability to navigate complex credentialing requirements while maintaining speed and accuracy has been a huge asset to our organization. We highly value their expertise and reliability. Derek Bravo CFO, Renew Health Renew Health has had the pleasure of partnering with Vanaa for over a year, and their impact on our organization has been exceptional. From the outset, their team has played a critical role in helping us navigate complex billing challenges; particularly around coding accuracy, timely resolution of denied claims, and proactively identifying and communicating operational roadblocks.
What sets Vanaa apart is their collaborative and solutions-oriented approach. They have worked seamlessly alongside our credentialing consultant, demonstrating both professionalism and a shared commitment to optimizing our revenue cycle performance. Their ability to operate as an extension of our internal team has been invaluable.
In 2026, our partnership has grown even stronger. Together, we have implemented a daily eligibility pipeline, established consistent bi-weekly reporting and strategy meetings, and gained greater visibility into key metrics such as participating and non-participating provider status, month-to-date and year-to-date payments, and aging claims across 0–120+ day buckets. These enhancements have significantly improved our financial oversight and operational efficiency.
Vanaa consistently goes above and beyond in their partnership with Renew Health. We are grateful for their collaboration and look forward to continuing to grow and expand our work together in 2026 and beyond.
Thanks AJay, Liz Smith Sr. Director Strategy & Operations AI-Augmented, human-led credentialing, so you can start billing sooner.

See What People Have To Say


Ready To Stop Credentialing Delays?
